Transform Your Healing with a Comprehensive Aftercare Support Program
Discover how your aftercare support program ensures seamless step-down care from PHP to lasting recovery.
Read MoreRecovering from addiction involves more than completing an inpatient or residential treatment program. An aftercare support program helps you navigate the critical transition from structured care to independent living. By offering continuing care, relapse prevention strategies, and ongoing guidance, these programs strengthen your coping skills and reduce the risk of relapse. Whether you engage in individual therapy, join a sober living home, or attend support groups, a comprehensive aftercare plan ensures you stay on track.
In this article, you’ll learn how to assess your aftercare needs, explore essential components of effective programs, and integrate structured services like partial hospitalization and intensive outpatient programs. You’ll discover steps to build a strong support network, develop relapse prevention plans, and sustain lifelong recovery. Let’s transform your healing with a robust aftercare support program.
Understand aftercare support
Define aftercare support
Aftercare, also called continuing care, refers to the lower-intensity services you receive following intensive treatment. These services bridge the gap between rehab and independent recovery. They may include therapy, medication management, sober living residences, and peer support. By maintaining connection with treatment professionals and peers, you reinforce the skills you gained during your initial treatment.
Connect to care continuum
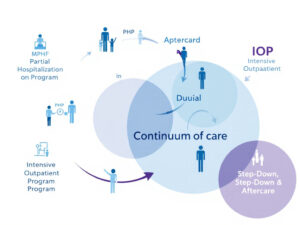
Your healing journey fits within a broader continuum of care addiction. This continuum typically moves from:
- Partial hospitalization
- Intensive outpatient programs
- Step-down care
- Aftercare services
Each level offers decreasing structure while preserving access to professional support. As you progress, aftercare ensures you have the tools and community to manage triggers in daily life.
Compare care levels
The table below summarizes how different care levels support your journey:
| Care level | Description |
|---|---|
| Partial hospitalization | Daytime treatment with clinical services and community integration partial hospitalization program |
| Intensive outpatient | Scheduled therapy sessions with flexibility to live at home intensive outpatient program |
| Step-down care | Transitional support combining therapy and supervised living step-down care program |
| Sober living homes | Peer-driven residences fostering accountability and shared routine |
Assess your aftercare needs
Identify relapse risk factors
Understanding your personal risk factors helps shape your aftercare plan. Common triggers include:
- Stressful life events
- Social pressures or old friend groups
- Co-occurring mental health disorders
- Gaps in daily structure
- Unresolved trauma
By pinpointing the emotional, mental, and physical stages of relapse, you can proactively address vulnerabilities before they lead to substance use.
Evaluate support gaps
Review the support you currently have at home and in your community. Ask yourself:
- Do you have reliable transportation to therapy?
- Are family or friends aware of your recovery goals?
- Is your living environment substance-free?
- Do you know where to turn for crisis assistance?
Identifying gaps allows you to seek structured aftercare services that fill those voids and provide tailored attention during vulnerable periods.
Align with recovery goals
Your aftercare plan should reflect your personal objectives. Whether you aim to return to work, rebuild family relationships, or pursue education, discuss how each component—therapy, support groups, sober housing—aligns with these goals. Customized recovery plans fuel continuous growth and adjustment as you advance in sobriety.
Explore aftercare components
Therapy and counseling
Ongoing therapy provides a safe space to explore emotions, refine coping strategies, and address co-occurring disorders. Key modalities include:
- Cognitive-behavioral therapy (CBT): Helps you challenge negative thought patterns and develop healthier behaviors
- Dialectical behavior therapy (DBT): Teaches emotional regulation and distress tolerance skills
Regular weekly sessions—gradually tapering as you build confidence—anchor your aftercare plan.
Peer support services
Connecting with peers who share lived experience bolsters motivation and accountability.
- Alumni programs: Former patients gather for events, sober activities, and phone check-ins
- Recovery community organizations: Local nonprofits offering coaching, outreach, and educational workshops
Evidence shows peer-led recovery support services can improve abstinence rates and overall wellbeing.
Medication management
If prescribed, medications like naltrexone, buprenorphine, or methadone help manage cravings and withdrawal symptoms. Your healthcare provider will monitor and adjust dosages to optimize safety and effectiveness.
Support group involvement
Twelve-step meetings (AA, NA) and alternatives such as SMART Recovery provide judgment-free environments, emotional support, and practical guidance. Regular attendance early in recovery significantly increases sustained sobriety.
Leverage structured support
Partial hospitalization benefits
A partial hospitalization program (PHP) offers intensive, day-level care without overnight stays. You receive:
- Medical evaluations
- Group and individual therapy
- Case management
PHP serves as a strong bridge if you need clinical support beyond residential treatment but still value daytime structure.
Intensive outpatient benefits
An intensive outpatient program or iop addiction treatment allows you to live at home while attending multiple therapy sessions per week. Key advantages:
- Flexibility to work or study
- Continued clinical oversight
- Peer support within structured sessions
IOP forms a core pillar of many aftercare plans.
Step-down care integration
A step-down care program merges supervised living with outpatient therapy. You transition gradually from high-intensity settings to independent life, reducing shock and reinforcing healthy daily routines.
Build a strong network
Engage family and friends
Your loved ones can play a pivotal role in recovery. Family therapy sessions and educational workshops help them understand addiction, communicate effectively, and support your objectives without enabling old patterns.
Involve professional providers
Maintaining relationships with clinicians ensures continuity of care.
- Counselors and therapists: Address evolving mental health needs
- Medical monitoring: Track medication management and physical wellness
Consistency in your care team enhances accountability and therapeutic rapport.
Connect peer mentors
Peer recovery coaches and sponsors provide mentorship rooted in firsthand experience. They offer hope, share practical strategies, and remind you that long-term recovery is achievable.
Develop relapse prevention plan
Recognize common triggers
List situations, feelings, and people that may tempt you to use. Awareness empowers you to intervene early and seek help when needed.
Apply HALT technique
Use the HALT framework—Hungry, Angry, Lonely, Tired—to check in with yourself regularly. Addressing these states proactively can defuse vulnerabilities before they escalate.
Create coping strategies
Develop healthy alternatives to substance use:
- Physical activity or yoga
- Mindfulness and meditation
- Creative outlets like art or music
- Structured daily routines
Test different approaches to find what works best for you.
Optimize your transition
Move from residential care
When leaving an inpatient setting, ensure you have a clear schedule of therapy appointments, support meetings, and sober living arrangements.
Enter outpatient programs
Enroll in a post rehab outpatient program or IOP right away to maintain momentum and clinical oversight.
Adjust to independent living
If you’re ready, consider sober living homes that offer peer accountability and a substance-free environment. These residences have proven to increase long-term sobriety chances.
Measure your recovery progress
Track key milestones
Celebrate achievements such as:
- 30, 60, 90 days sober
- Completing therapy goals
- Rebuilding healthy relationships
Documenting successes reinforces your commitment.
Review and adjust plan
Recovery isn’t linear. Periodically revisit your aftercare components and tweak session frequency, living arrangements, or coping tools based on what’s effective.
Gather ongoing feedback
Stay open with your care team and sponsors. Honest feedback guides you toward resources or adjustments that enhance your path.
Sustain lifelong recovery
Embrace continuing care
Aftercare isn’t indefinite, but ongoing check-ins—monthly therapy or periodic alumni events—help you maintain focus and accountability.
Participate in alumni activities
Attend sober outings, workshops, and reunions organized by your treatment center or community groups. These events renew connections and combat isolation.
Prepare emergency responses
Develop a crisis plan that includes:
- Who to call in a moment of intense craving
- Favorite coping exercises
- Quick-access hotline numbers
Having this roadmap at hand ensures you respond rather than react under stress.
By engaging in a structured, comprehensive aftercare support program, you strengthen your foundation for lasting recovery. Through therapy, peer support, sober living, and ongoing monitoring, you’ll navigate life’s challenges with confidence and resilience. Remember, sustained sobriety is built one day at a time, backed by the right tools and a supportive network.