Why the Rehab Intake Process Is Key to Your Treatment Success
Discover why the rehab intake process matters and how it guides you through admissions, costs, and coverage.
Read MoreUnderstanding the rehab intake process
When you think about starting rehab, you might picture therapy sessions, group meetings, or a private room where you can finally rest. Before any of that begins, you go through something equally important: the rehab intake process.
The rehab intake process is the structured series of steps that helps a treatment team understand your history, your health, your goals, and your practical needs. This is where you share your story, your concerns about cost and insurance, and what you want your life to look like after treatment.
Programs that take intake seriously use it to build a personalized recovery plan, not a one size fits all schedule. At many centers, this includes gathering information about your substance use history, medical background, mental health, family dynamics, and personal goals so your care can be tailored from day one [1].
Understanding how this works can reduce anxiety, help you ask better questions, and make it easier to move from thinking about treatment to actually starting it.
Why intake is so important for treatment success
The rehab intake process is not just paperwork or a simple admissions step. It is the foundation of your entire treatment experience. When intake is done thoroughly and thoughtfully, it affects almost every aspect of your recovery.
It shapes a personalized treatment plan
During intake, clinical staff gather detailed information about:
- What you use, how often, and for how long
- Your physical health and medications
- Your mental health history and current symptoms
- Your family situation and support system
- Any previous treatment or recovery attempts
This information allows doctors, therapists, counselors, and wellness practitioners to collaborate on a treatment plan that fits you, not just your diagnosis. After intake, many programs build a plan that can include specific therapies such as cognitive behavioral therapy, relapse prevention strategies, and medical support, with ongoing adjustments as you progress [2].
A strong intake process means your care can be fine tuned as you move through detox, inpatient or outpatient services, and aftercare.
It protects your safety from day one
If you are using alcohol, opioids, benzodiazepines, or multiple substances, stopping suddenly can carry real medical risks. During rehab intake, clinicians assess:
- Your risk of withdrawal complications
- Any co occurring medical conditions
- Current medications or health concerns
Upon arrival, a comprehensive medical and psychological evaluation is often completed to identify withdrawal risks and decide if medical detox is needed before you participate in therapy [3].
This is critical for your safety and comfort. If you need detox, it will be built into your plan and monitored by a medical team, ideally in a private, calm environment where you can stabilize.
It addresses practical barriers early
A major reason people hesitate to enter treatment is worry about cost, insurance, and logistics. A well designed rehab intake process addresses these from the beginning instead of leaving you guessing.
Admissions and financial counselors typically:
- Verify your insurance and explain what is covered
- Estimate out of pocket costs
- Offer or discuss payment plans
- Explore financial assistance or government funded programs such as Medicaid when appropriate [2]
By tackling these issues head on, intake can remove some of the biggest obstacles to getting help.
Step one: Initial contact and pre screening
Your rehab intake process usually starts before you ever walk through the door.
Reaching out for the first time
The first step is often a phone call or online inquiry with an admissions specialist or navigator. During this conversation you may be asked about:
- Basic contact information
- What you are using and how often
- How severe things feel right now
- Any urgent medical or mental health concerns
- Your motivation for treatment
- Your insurance information
Centers use this to determine urgency and the appropriate next steps [3]. If you are in crisis, they may direct you to immediate medical care before formal intake.
If you want to understand how this looks at a specific facility, you can often review their process on pages about admissions for rehab and then call to ask detailed questions.
Clinical pre admission assessment
After the initial contact, a licensed counselor or clinician may conduct a more detailed pre admission assessment. This is typically done by phone and focuses on:
- Medical history and current conditions
- Mental health history and any diagnoses
- Substance use patterns, including type, amount, and duration
- Withdrawal symptoms you may have experienced
- Impact of substance use on relationships, work, or school
This information helps staff decide on the right level of care, for example detox, residential, or intensive outpatient, and identify any co occurring disorders that need simultaneous attention [2].
When this step is handled with compassion and without judgment, it can also reassure you that you will be seen as a whole person, not just as an “addict.”
Step two: Insurance verification and cost planning
Once a program understands your clinical needs, the next question is usually cost. The rehab intake process builds in a clear, structured way to address this.
Checking your insurance benefits
Insurance verification typically happens early, often within 24 to 48 hours, and can be expedited when needed [1]. During this step, admissions or billing staff contact your insurer to confirm:
- What levels of care are covered, for example detox, residential, outpatient
- Any prior authorization requirements
- Your deductible and coinsurance
- Any limits on length of stay
Many private and public insurance plans cover at least part of rehab, including major insurers and some Medicaid programs [4]. If you are not sure whether your plan is accepted, you can use tools such as verify insurance for treatment or review insurance coverage for treatment on the facility’s site.
Some centers also highlight themselves as an insurance accepted rehab. This can give you a starting point if you are comparing programs.
Building a realistic payment plan
After insurance is verified, the financial counseling part of intake helps you understand:
- Your estimated out of pocket costs
- What portion insurance is expected to pay
- Whether payment plans are available
- Options for help if you are underinsured or uninsured
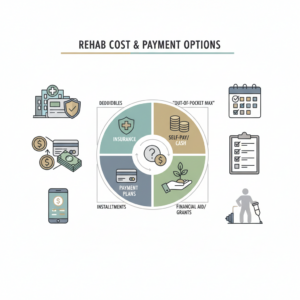
Many rehab admissions teams assist with flexible payment plans and can connect you with financial assistance or state funded programs to make treatment more affordable [2]. For more detail on how this might work in practice, you can review resources such as rehab cost and payment options and financing rehab programs.
Knowing this information before you arrive helps reduce stress and lets you focus on recovery instead of financial uncertainty.
A clear, transparent financial discussion at intake can be the difference between delaying treatment and starting it with confidence.
Step three: Arrival, orientation, and evaluations
Once you have completed pre screening and financial planning, you move into the on site portion of the rehab intake process.
Medical and psychological evaluations
Upon arrival, you are usually welcomed by staff and then guided through a thorough assessment process. This typically includes:
- A full medical evaluation
- A psychological and biopsychosocial assessment
- A detailed substance use and withdrawal risk evaluation
These assessments are often completed by multiple specialists so that the team has a complete picture of your needs [2]. The goal is to make sure you are safe, stabilize any urgent issues, and confirm whether you need closely monitored detox before you begin the core treatment program.
If you have co occurring mental health issues such as depression, anxiety, or trauma related symptoms, this is where they are formally identified and built into your plan.
Orientation to the environment
Orientation usually covers:
- A tour of the facility, including your room and common spaces
- Explanation of daily schedules and rules
- Introduction to key staff and your primary therapist or case manager
- How to access medical support or ask for help
If you are considering a private rehab facility, this is also when you see how privacy and comfort are handled in practice. Many clients appreciate private or semi private rooms, quiet spaces, and clear boundaries to support rest and reflection. Some centers even allow you to tour residential rehab virtually or in person before you commit, so you know what to expect on arrival.
How intake addresses common barriers to treatment
Even when you are motivated to change, it is common to face internal and external barriers. A research review of substance use disorder treatment identified dozens of structural, individual, and social obstacles that can delay or prevent people from starting care [5]. The rehab intake process is a chance to address many of these directly.
Structural and financial barriers
Structural barriers include limited access to services, insurance challenges, and policy restrictions, such as a lack of skilled providers or rigid institutional rules [5]. Intake teams can help by:
- Navigating insurance coverage and authorization
- Offering flexible scheduling where possible
- Connecting you to state funded or sliding scale programs when needed
- Coordinating care across different providers
Supportive policies, good management, and flexible program design have all been identified as key facilitators for better access to treatment [5].
Individual fears and misconceptions
On a personal level, many people delay treatment because of fear or mistaken beliefs. For example, some believe they can manage withdrawal alone or assume rehab will not work for them. These wrong beliefs, combined with psychiatric symptoms such as anxiety or depression, can reduce motivation to seek help [5].
During intake, clinical staff can:
- Explain what detox and treatment really involve
- Clarify safety measures and medical support
- Talk through your prior experiences with treatment, good or bad
- Help you set realistic expectations and personal goals
This clear, honest conversation can reduce fear and replace guesswork with concrete information about what will happen next.
Social stigma and lack of support
Social level barriers include stigma, lack of family support, and negative experiences with past providers [5]. Intake offers a structured moment to invite supportive family members into the process, with your permission, and to reset the tone of how professionals engage with you.
Many programs encourage a trusted loved one to join part of the intake discussion. This can help:
- Correct misinformation about rehab
- Align expectations and boundaries
- Build a shared understanding of what recovery will require
When done well, the intake process begins to replace shame with understanding and isolation with connection.
External resources that can help you start
If you are unsure where to begin, you do not have to figure out the rehab intake process on your own.
National helplines and referrals
SAMHSA’s National Helpline provides free, confidential treatment referral and information 24 hours a day, 7 days a week, in English and Spanish, for people and families facing mental and substance use disorders. The specialists do not offer counseling, but they connect you to local treatment facilities and support groups and help you find appropriate intake centers in your area [6].
You can also text your 5 digit ZIP code to 435748 (HELP4U) to receive referrals to nearby services. This text based option is currently available in English and can be especially helpful if you are not ready to talk on the phone [6].
The service does not require insurance and can link you to state funded programs or facilities with sliding fee scales, which expands your options at the intake stage [6]. Importantly, they do not ask for identifying personal details beyond your location, so your privacy is preserved.
What intake looks like in different types of programs
Not every rehab program is identical, but the core elements of intake show up in most settings.
Residential or inpatient rehab
In a residential setting, intake is typically more extensive because staff are responsible for your care 24 hours per day. You can expect:
- On site medical exams and lab tests when needed
- Detailed psychological and social evaluations
- Care planning that includes housing, room assignment, and daily structure
If you are entering a program with private rooms, intake is also where you learn about any room preferences, roommate policies if applicable, and how privacy is protected.
Outpatient and intensive outpatient programs
With outpatient care, intake still includes clinical and financial assessments, but logistics focus more on scheduling, transportation, and how to integrate treatment into your daily life. Your intake team will discuss:
- How many days and hours you will attend each week
- How sessions fit with work or family obligations
- Remote or telehealth options when available
The goal is the same, to create a plan that you can realistically follow and that addresses both substance use and mental health needs.
How to prepare yourself for the rehab intake process
You do not need to have everything figured out before you start intake. However, a bit of preparation can make the process smoother and more productive.
Consider gathering:
- A list of medications you are taking
- Any recent medical records or diagnoses
- Your insurance card and basic plan details
- Contact information for key family members or supporters
It can also help to think about your goals. You might ask yourself:
- What do you want to be different six months from now
- Are there specific relationships you want to repair
- What has helped or hurt your recovery efforts in the past
Bringing these reflections into intake gives your treatment team more to work with as they build your plan.
Using intake to advocate for your needs
The rehab intake process is not a one way interview. It is also your chance to ask questions and advocate for what matters to you.
You can use this time to clarify:
- How the program handles privacy and confidentiality
- Whether private or semi private rooms are available
- How family involvement is structured
- What your daily schedule might look like
- How the program measures progress and success
Intake is also the right place to disclose any accommodations you might need, such as support for mobility challenges, dietary needs, or religious practices. The more accurately you describe what you need, the better your team can design a plan that supports you.
Bringing it all together
When you look closely, the rehab intake process touches almost every factor that influences your treatment success. It informs your clinical care, protects your safety, clarifies your financial responsibilities, and begins to dismantle the barriers that kept you from treatment in the first place.
By understanding each step, from initial contact and insurance verification to medical evaluation and orientation, you can approach intake with more confidence and less fear. If you are ready to explore your options, you can review admissions for rehab, check an insurance accepted rehab, or use tools to verify insurance for treatment and review rehab cost and payment options.
Taking that first step into the intake process is not just administration. It is the beginning of a structured, informed path toward recovery that is built around you and your goals for the future.